29 The Untold Message of Breast Cancer Awareness Month by Jeffrey Dach MD
by Jeffrey Dach MD
__________________________________________
Breast Cancer Awareness Month Fails to Disclose Limitations of Mammography
 October was Breast Cancer Awareness Month, which is an advertising campaign for national mammography screening. (1)
An eminent radiologist, Leonard Berlin MD says this advertising message
fails to disclose the limitations of screening mammography, namely that
mammography will miss 30-70% of breast cancers, and leads to over
diagnosis and over treatment. He also says mammography disclosures
should be mandated, just like the cigarette and drug warnings that
appear on their ads.(2)
Otherwise, we create unrealistic expectations for mammography which
cannot be met. The public expects every breast cancer to be detected.
They are not. This translates into increased medical malpractice payouts
for the missed cancer, which is now the most prevalent medical
malpractice case against all physicians.(3)(4)(5)(6)
October was Breast Cancer Awareness Month, which is an advertising campaign for national mammography screening. (1)
An eminent radiologist, Leonard Berlin MD says this advertising message
fails to disclose the limitations of screening mammography, namely that
mammography will miss 30-70% of breast cancers, and leads to over
diagnosis and over treatment. He also says mammography disclosures
should be mandated, just like the cigarette and drug warnings that
appear on their ads.(2)
Otherwise, we create unrealistic expectations for mammography which
cannot be met. The public expects every breast cancer to be detected.
They are not. This translates into increased medical malpractice payouts
for the missed cancer, which is now the most prevalent medical
malpractice case against all physicians.(3)(4)(5)(6)Left Image: Giant pink ribbon on the corner of 5th and Market, downtown Louisville, KY (10-5-06) Source Breast Cancer Awareness Jason Meredith from Louisville, KY, US Courtesy Wikimedia Commons
The fact is that mammograms are difficult to interpret, cancers can be hidden, and many are missed. This cancer miss is not from lack of training or competency on the part of the radiologist. It is inherent in the mammogram technique itself. The American College of Radiology says that 30-70% of breast cancers are missed on the initial mammogram, and are seen in retrospect a year later by going back to the previous mammogram interpreted as normal.With this legal environment, it is a miracle that mammography has survived at all.(7)(8)
Screening Mammography is Not Prevention.
 Leonard
Berlin points out that 57% of the American women believe that
mammograms prevent breast cancer, a misleading message from Breast
Awareness Month.(3)
Leonard
Berlin points out that 57% of the American women believe that
mammograms prevent breast cancer, a misleading message from Breast
Awareness Month.(3)Left Image: Woman undergoing a mammogram of the right breast Source US National Institutes of Health - National Cancer Institute
Mammograms are designed to detect cancer, not prevent it. Thinking that a mammogram can prevent breast cancer is like thinking that checking your house annually for broken windows, prevents robberies.
Secondly. the most likely outcome of a positive mammogram is an unnecessary biopsy, causing emotional distress, breast deformity and scarring. 80% of all breast biopsies done for a positive finding on a mammogram are negative for cancer.(7)
My Own Experience with Mammography
When I began residency training in radiology at Rush Presbyterian Hospital in Chicago in 1971, the state of the art was Xeromammography. This was a machine made by the Xerox Company which was prone to mechanical failure, and always breaking down. It produced a blue photo on paper with blue toner powder.(9)

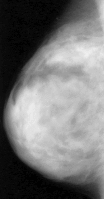
Xerox Type Xray Mammogram
Useful to the Surgeon
In those early days, the surgeon's criteria for doing a breast biopsy was a palpable mass. Many women have palpable lumps and bumps called fibrocystic breast disease which is quite common, and now known to be caused by iodine deficiency.(12)
Cyst or Solid Breast Mass?
In those days, the surgeon approached a breast mass with needle aspiration to differentiate between a fluid containing cyst or a solid mass. Nowadays, ultrasound determines this easily.
Back to the needle aspiration procedure; if the lesion is a cyst, the fluid is removed and the mass disappears. If no fluid can be obtained, then the mass is solid, and surgical removal is the next step. This is where the surgeons found the xeromammogram useful, occasionally showing a second occult mass or calcification which alerts the surgeon to remove additional tissue.
Invention of Needle Localization
Sometimes the surgeon had trouble actually finding the tiny calcifications at surgery since they could not feel them, so needle localization was invented. The radiologist placed a needle in the breast tissue near the calcifications which guided the surgeon to the spot to be removed. The surgically excised breast tissue was returned to the X-ray department for another mammogram of the specimen to determine if the lesion had been removed (see below).
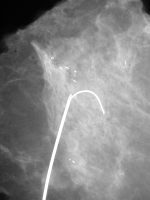

Left Image: Excised specimen with needle localization (done for calcifications)
Right Image: Needle Localization for spiculated mass typical for malignancy in specimen.
The Switch from Blue Paper to Gray Xray Film
Grey X-Ray film mammograms replaced the blue Xerox paper images around 1982. By that time, I had joined a radiology group in Hollywood, Florida, but they were still using the xerox machine even though the whole country had already made the switch to regular x-ray film. This inevitable switch-over to X-ray film made possible the large scale national breast screening programs, since the mammogram could be done at any hospital x-ray department.(9)
Finally, We All Learn Mammography
My radiology group made the plunge into film mammography. None of us had prior training or experience reading mammograms, so we traveled to expensive meetings and teaching courses on mammography from leaders in the field, such as Marc Homer MD and Laszlo Tabar MD (Sweden), and then we started reading on our own.(57)(13)
From Breast Needle Biopsy to the Creation of a New Department
Soon we were doing the needle localizations using the Marc Homer needle, and needle biopsies in the radiology department. Initially, biopsies were done simply with a standard 20 gauge needle and 10 cc disposable syringe. A few years later, the radiology industry came out with spring loaded and vacuum assisted biopsy guns, and later invented dedicated biopsy tables using stereo-tactic guidance. This stereo guided machine allows the operator to take two x-rays at different angles, and uses a computer to calculate the exact depth and angle to advance the biopsy needle into the breast lesion.
By 2005, the cranky unreliable blue toner xeromammogram had been replaced with a shiny new department on the third floor with all the new modalities of hi-resolution digital mammography, stereotactic biopsy, breast ultrasound, and breast MRI. There is no question that the combination of these modalities makes a powerful and useful tool for diagnosis, treatment and follow up of breast cancer cases.
Screening is Quite Different from the Diagnostic Mammogram
However, screening mammography is quite different from diagnostic mammography as discussed below. Diagnostic mammography deals with a known abnormality in the breast, a mass or a palpable lump or even an abnormality on a breast thermogram or any suspicious area. In this case, the mammogram is quite useful in evaluating the abnormality to determine if it represents cancer. Screening mammography, on the other hand, takes a population of the worried well, and submits them to a mammogram to screen for any abnormality which might turn out to be cancer.
Victimization of Women?, No, Merely Good Medical Care.
When the screening mammogram program started years ago, many of the suspicious findings were false positive meaning they looked like something, but were in fact nothing. The radiologist would send a report of "suspicious requires biopsy" to the doctor who would tell the patient it might be cancer, and the terrorized woman would then not only submit to surgical biopsy under anesthesia, she would become hysterical and insist on the biopsy immediately. A negative biopsy would be then be a relief to the patient, also turning the surgeon into a hero. Feminists call this victimization of women, and healthcare professionals would call this good medical care.
Occasionally, about 10-20% of the time, a real cancer would be found at surgery. These were typically spiculated masses or fine branching calcifications. In the early days, the punctate calcifications and the milk-of calcium (teacup calcium) were called benign and did not require biopsy, and the branching calcifications indicated malignancy requiring biopsy and further treatment. However, nowadays, even the benign calcifications are routinely sent for biopsy, sometimes showing a controversial non-aggressive cancer called DCIS. (14)(15)
What's Your Track Record ?
At first, we had no idea how many of our mammogram readings of suspicious for cancer were actually found to be cancer by surgical biopsy and pathology evaluation. So to answer this question, we started compiling the pathology data and attended monthly conferences to review the data and our track record. We found that on average, one cancer for every 5 biopsies, but each radiologist and hospital may have more or less. Optimally, this information should be posted on the wall of the waiting room. Unfortunately, this type of data is rarely available to the patient.
Questioning Screening Mammography
 In
the 1980s everyone in health care believed that mammography was capable
of early detection of breast cancer, and that mass screening programs
were capable of reducing breast cancer mortality. I also believed in
this, and to show my loyalty, I wrote an editorial in the Miami Herald
praising the merits of screening mammographyis which won the admiration
of my colleagues in the radiology department.
In
the 1980s everyone in health care believed that mammography was capable
of early detection of breast cancer, and that mass screening programs
were capable of reducing breast cancer mortality. I also believed in
this, and to show my loyalty, I wrote an editorial in the Miami Herald
praising the merits of screening mammographyis which won the admiration
of my colleagues in the radiology department.However, beginning in 1995, I began to have doubts and misgivings and began to question the value of screening mammography. Right from beginning days, a debate raged between the advocates and the critics of screening mammography, arguing that medical studies of the technique either did, or did not show reduction in breast cancer mortality. Some critics of mammography screening such as Samuel Epstein MD say that mammograms cause harm from overtreatment with unnecessary breast biopsies, and the radiation exposure increases breast cancer risk.(24)(25)(26)(27)(28) Other outspoken critics such as Nortin Hadler(37) , Michael Baum (46)(47)(48)(49(50)) and David Plotkin (39) have said screening mammography is so blunt that it approaches being useless, finding very few cancers that are truly treatable, and missing many of these, and it produces too many false positives. They seriously doubt that screening mammography has any impact on breast cancer mortality.
Luck of the Draw - Mammography Malpractice
One of radiologists in my group had the misfortune of being sued for malpractice. He missed a cancer on a mammogram that was visible in retrospect a year later. Remember, this routinely happens 30-70% of the time. This event happened early in his career, just out of his training period, before I met him. The story I heard was that the insurance company quickly settled the case by paying the woman a settlement of a million dollars, with no attempt at defending the case. As you can imagine, this was a major event which changed how my partner interpreted mammograms. After that event, it was understandable that he was gun shy, and almost always called the patient back for additional mammograms, and always recommended biopsy for any vague density. The problem is that almost every mammogram has vague densities, and almost all of the biopsies recommended under such circumstances are unnecessary for the patient, but are quite necessary for the radiologist, considering the medico-legal climate aptly described by Dr. Leonard Berlin.(3)
It quicky became a game where the x-ray technologists learned to bring the mammograms over to my side of the room to my reading area for a quick negative report, rather than to the other side of the reading room, where they can bet on doing additional mammogram views, and then have the patient sent for a biopsy of a questionable area. We played this game many years, and even with all these negative reports, I was never sued for malpractice for a mammogram reading during my entire career. I consider this "the luck of the draw".
Realizing the high rate of false positive biopsies and the emotional impact on women, I did my best to call the negative mammograms negative, all the while acknowledging there could be a cancer hiding on the mammogram somewhere, perhaps underneath an area of vague density. That was just one of the limitations of mammography. At the same time, when I did see abnormalities that had a high probability of cancer, these bonafide cases were sent for breast biopsy for good reason.
Biopsy Everything and Anything
The reality of a hostile medico-legal malpractice climate and the financial pressures dictates the practice of mammography in most community hospitals. This basically means that the usual practice is to biopsy anything and everything that shows up on the mammogram, as long as the patient is compliant. It is not difficult getting compliance by telling patient that it might be cancer, we just can't be sure. That usually is enough to make the woman hysterical and submit to biopsy. The radiologist is happy because he thinks he is reducing his chances of being sued for malpractice. His partners and the hospital administrators are happy because the procedures bring in more income. If cancer is found, the surgeons are happy because they have more lumpectomies and cancer operations to keep them busy.
DCIS, the Controversial Non-Aggressive Cancer
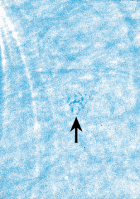
Over half of the cancers detected with mammography are DCIS (ductal carcinoma in situ). This is a non-aggressive form of cancer which has a 98% survival after 5 years even with no treatment, although when found, the DCIS cases are treated with surgery just like any other cancer.(31) Some consider this detection and treatment of DCIS a form of overtreatment, others consider it good medical care.
 Some
critics have said that increased mammographic detection of DCIS has
skewed the statistics, falsely reducing breast cancer mortality. This
makes it look like we are reducing breast cancer mortality, while in reality there is no reduction in mortality from the real breast cancers.(33)
Some
critics have said that increased mammographic detection of DCIS has
skewed the statistics, falsely reducing breast cancer mortality. This
makes it look like we are reducing breast cancer mortality, while in reality there is no reduction in mortality from the real breast cancers.(33)Left Image: Small calcifications representing DCIS (arrow) on an old Xerox-mammogram.
Without mammography, most of these DCIS cases would go undetected, and probably never cause a problem. Autopsy studies of women dying from car accidents have shown occult DCIS in up to 15% of the population.(16)(17) The actual incidence of cancer mortality is 0.4 per cent, not 15 per cent, suggesting that 96% of DCIS cases never go on to clinical disease. Yet, when DCIS is detected on the mammogram, these cases are treated with the same mastectomy or lumpectomy. A third of the time, pathologists will disagree on the diagnosis of DCIS while looking at the same case.(16)(17)
Lung Cancer Screening
 Screening
tests in radiology have been tried before. For example chest x-ray
screening for lung cancer was tried, studied and abandoned. It was found
that when you do a chest X-ray on smokers every 6 months, find the
cancers and send the patient to surgery for treatment, there is no
change in mortality figures. No lives are saved. In addition to make
matters worse, when you go back to the earlier films 6 months before, on
the film that was read as negative or normal in retrospect the lesion
is visible 90% of the time.(18)
Screening
tests in radiology have been tried before. For example chest x-ray
screening for lung cancer was tried, studied and abandoned. It was found
that when you do a chest X-ray on smokers every 6 months, find the
cancers and send the patient to surgery for treatment, there is no
change in mortality figures. No lives are saved. In addition to make
matters worse, when you go back to the earlier films 6 months before, on
the film that was read as negative or normal in retrospect the lesion
is visible 90% of the time.(18) Left Image: Small Lung Cancer in Black Box on Chest Xray Courtesy of Wikimedia
We thought these problems would be solved by moving up to CAT scans, a more advanced imaging technique. However, now we have a problem with seeing too many "suspicious" lesions and the false positive diagnosis. The net result is that lung cancer screening even with CAT scanning has not caught on.(19)
Mammogram screening in the under 50 age group NOT recommended by all other countries.
Current guidelines recommend a screening mammogram every 2 years for the 40-50 year age group. No other western country does this, as these women have dense breast tissue difficult to image and are most prone to a false positive reading, or a diagnosis of DCIS, the controversial less aggressive form of cancer. Most European countries restrict screening to post-menopausal women, after 50, when breast tissue involutes to fat and the cancers become more conspicuous.
Efficacy of Breast Cancer Screening - Does It Reduce Mortality?
The public perception is that breast cancer screening reduces breast cancer mortality. The reality is that this is a fiercely debated question in the medical literature with no clear winner. Leonard Berlin's articles summarize this debate in the medical literature.(5)
The debate is best shown by one example mentioned Dr. Berlin in the Sept 2002 issue of the Annals of Internal Medicine in which two conflicting articles appeared in the same issue, one stating that mammography has no mortality benefit, and the other saying it does.
Here are the Two Opposing Views on Mortality Benefit:
(1) Canadian researchers concluded that mammography screening did not reduce breast cancer mortality.(20)(21)
(2) United States Preventive Services Task Force concluded mammography reduces breast cancer mortality among women 40-74 years old.(22)(23)
Another excellent review of major Mammography Screening Studies can be found at the National Breast Cancer Coalition.(59)(24)
Bottom line, the debate rages on with no clear winner.
One observation which might clarify the debate is this: in two countries with socialized medicine, Canada and Sweden, careful studies of mammography screening were found to have NO Mortality Benefit compared to breast clinical exam.
Here in the US, however, with a 4 billion dollar fee-for-service screening mammogram industry, the mammography studies are interpreted to show that Yes, there is a Mortality Benefit of about 15-20% .
The influence of money and politics over medical science is pervasive, and mammography is certainly not immune. A few MD PHD's from Canada or Sweden are not about to derail a 4 billion dollar industry in the US.
Conflict of Interest in Sponsoring Breast Cancer Awareness Month?
Screening mammography critic, Samuel Epstein MD, irritates the establishment every time he points out that in 1984, the American Cancer Society created the October National Breast Cancer Awareness Month sponsored by money from the Astra-Zeneca Company, the maker of Tamoxiphen, the best selling breast cancer drug. In addition, Astra-Zeneca also manufactures industrial chemicals that cause breast cancer. Some consider this a conflict of interest.
Epstein also points out that past ACS advertisement promised early detection results in a cure nearly 100% of the time. Even more seriously, the Awareness Month advertisements avoid any reference to information on avoidable causes and prevention of breast cancer.(24)(25)
What is breast cancer prevention?
A previous newsletter discusses Iodine supplementation as the most effective way to prevent breast cancer. Iodine tablets are safe, inexpensive and readily available. This is true prevention.(12)
Samuel Epsteins landmark book, "The Politics of Cancer" discusses carcinogenic chemicals in our food supply, home and workplace. Removing them can reduce breast cancer. This is true prevention.(26)(27)
The Untold Message of Breast Cancer Awareness Month:
To summarize, here is the untold message of Breast Cancer Awareness Month:
1) mammography screening is detection, not prevention and has several limitations, namely 30-70% missed cancers, and a tendency towards over diagnosis and over treatment.(7)
2) Many different carcinogenic chemicals cause breast cancer, and removing these chemicals from the workplace or home can reduce breast cancer rates. (26)(27)
3) Iodine deficiency causes fibrocystic disease, and Iodine supplementation prevents breast cancer.(12)
4) Synthetic hormones like Provera increase breast cancer risk. (WHI Study)(29)
5) Bio-Identical Hormone programs are safe, and do not increase risk of breast cancer. (French Cohort Study)(30)
Will mainstream medicine ever endorse Dr. Leonard Berlin's Truth-in-Mammography disclaimers? I predict this will never happen. Instead, the public's unrealistic expectation that a breast cancer nodule will be detected 100% of the time will continue, and the high cost of medical malpractice will simply be absorbed into "the cost of doing business". The screening mammogram is here to stay. As for my opinion, I am not opposed to the status quo of mammogram screening in the over 50 age group. However, we should educate the public to be realistic in their expectations of mammography. Unfortunately this task of educating the public is thwarted by the unrealistic expectations created by false and deceptive advertising about screening mammography. Perhaps that is the untold message of October Breast Cancer Awareness Month.
Articles with related content
Iodine Supplementation and Breast Cancer Prevention
PSA Screening for Cancer, the Failed Medical Experiment by Jeffrey Dach MD
The Thyroid Nodule Epidemic by Jeffrey Dach MD
Jeffrey Dach MD
7450 Griffin Road Suite 190
Davie Fl 33314
www.jeffreydachmd.com
www.drdach.com
www.naturalmedicine101.com
www.truemedmd.com
BLOG
TrueMedMD
disclaimer
References
(1) http://www.cancer.org/docroot/PED/content/PED_2_3X_ACS_Cancer_Detection_Guidelines_36.asp?sitearea=PED
American
Cancer Society Breast Cancer Prevention Page: Yearly mammograms are
recommended starting at age 40 and continuing for as long as a woman is
in good health.
(2) http://www.rnsmc.org/news_article.asp?ID=41
Leonard
Berlin, M.D, FACR, Chairman of Radiology at Rush North Shore Medical
Center, Skokie, was awarded the Distinguished Service Gold Medal Award
of the Chicago Radiological Society, its highest honor on April 21,
2005 in Chicago, IL. The Gold Medal is awarded annually to an individual
who has rendered unusual service to the science of radiology and will
be presented to Dr. Berlin by his son, radiologist Jonathan W. Berlin,
M.D. Berlin is Charman of Skokie Valley Hospital Department of
Radiology.
(3) http://radiology.rsnajnls.org/cgi/reprint/233/3/641
Mammography
Screening Can Survive Malpractice . . . If Radiologists Take Center
Stage and Assume the Role of Educator by Leonard Berlin, MD. Radiology
December 2004.
(4) http://www.ajronline.org/cgi/content/full/176/5/1131
The
missed breast cancer redux: time for educating the public about the
limitations of mammography? Berlin L. AJR 2001; 176:1131-1134
(5) http://www.ajronline.org/cgi/content/full/180/5/1229
Malpractice
Issues in Radiology, Breast Cancer, Mammography, and Malpractice
Litigation: The Controversies Continue Leonard Berlin, AJR 2003; 180:1229-1237, Excellent discussion of controversy of screening mammography and impact on mortality figures.
(6) http://www.ajronline.org/cgi/content/full/176/5/1123
Perspective
on Dot Size, Lead Time, Fallibility, and Impact on Survival Continuing
Controversies in Mammography Leonard Berlin MD. AJR 2001; 176:1123-1130
(7) http://www.fda.gov/ohrms/dockets/ac/03/briefing/3945b1_05_Berlin%20testimony.pdf
STATEMENT
of Leonard Berlin, M.D. To the U.S. Senate Committee on Health,
Education Labor and Pensions Re: Mammography Quality Standards Act
Reauthorization April 8, 2003. Leonard Berlin: Suffice it to say that
research studies performed at some of the most prestigious medical
institutions in the United States reveal that as many as 90% of lung
cancers, and 70% of breast cancers, can at least partially be observed
on previous studies read as normal.
(8) http://www.imagingeconomics.com/issues/articles/2004-11_02.asp
A
Manifesto for Truth-in-Mammography Advertising by Leonard Berlin MD
Imaging Economics, November 2004. "From cigarettes to pharmaceuticals to
financial services, all advertisements feature a disclaimer: Why not
those for mammography? Of all medical malpractice lawsuits filed in the
United States that allege a delay in the diagnosis of breast cancer,
radiologists are the most frequently sued specialists. Of all medical
malpractice lawsuits lodged against radiologists, the most frequent
cause is the allegation of a missed breast cancer on mammography. Why
has "missed breast cancer" risen to first place in the medical
malpractice standings? I suggest that it is because we have oversold
mammography. We have marketed mammography without informing the American
public all that we know about not only the benefits, but more important
the limitations and potential harms of mammography."Endquote.
(9) http://radiology.rsnajnls.org/cgi/content/full/215/1/1
Breast
Imaging: From 1965 to the Present Edward A. Sickles, MD, Radiology.
2000;215:1-16.) Examples of xeromammograms and film mammograms,
speculated lesion, needle localization.
(10) http://www.chi-rad-soc.org/illinois.html
History:
Narratives Radiology in Illinois By Franklin Alcorn, M.D. Dr. Alcorn's
history appeared in the program of the Chicago Radiological Society at
the Centennial of Radiology in 1995.
(11) http://www.chi-rad-soc.org/illinois.html
History:
Narratives Radiology in Illinois By Franklin Alcorn, M.D. Dr. Alcorn's
history appeared in the program of the Chicago Radiological Society at
the Centennial of Radiology in 1995.
(12) http://jeffreydach.com/2007/05/05/jeffreydachdrdachiodine.aspx
Breast
Cancer Prevention and Iodine Supplementation by Jeffrey Dach MD,
Iodine Supplementation Prevents Breast Cancer by Jeffrey Dach MD
(13) http://www.sma.org/AM2005/ANM2004pdfs/Saturday/S21_Otto_P.pdf
Screening
mammogram Swedish Study by Dr. Laszlo Tabar (1977- 1984)
Population-based randomized controlled study showed 31% reduction in
breast cancer mortality in women 50 plus. Breast Cancer Screening
Southern Medical Association’s 98th Annual Scientific Assembly November
13, 2004 Pamela M. Otto, MD Associate Professor UTHSCSA, Dept of
Radiology
(14) http://sprojects.mmi.mcgill.ca/mammography/calcifications1.htm
INTERACTIVE
MAMMOGRAPHY ANALYSIS WEB TUTORIAL. Images of benign calcifications,
secretory disease, milk of calcium, etc. Molson Medical Informatics
Project 1999. McGill University.
(15) http://sprojects.mmi.mcgill.ca/mammography/calcifications3.htm
Tutorial 2 : CALCIFICATIONS ASSOCIATED WITH A HIGH PROBABILITY OF MALIGNANCY
Molson
Medical Informatics Project 1999. McGill University. Fine linear
branching calcifications are high probability for malignancy.
(16) http://www.moffitt.org/moffittapps/ccj/v6n3/article5.htm
Ductal
Carcinoma In Situ of the Breast by Elisabeth L. Dupont, MD; Ni Ni K.
Ku, MD; Christa McCann, BA; and Charles E. Cox, MD, FACS. Moffitt Cancer
Center. DCIS, 60% of DCIS cases are discovered solely by mammography.
Seven major autopsy studies of women not known to have had breast cancer
have provided insight. Six studies found an incidence of 4% to 18%.
DCIS now accounts for nearly half of mammographically detected cases of
cancer.
(17) http://www.annals.org/cgi/content/full/127/11/1023
Using
Autopsy Series To Estimate the Disease "Reservoir" for Ductal Carcinoma
in Situ of the Breast: How Much More Breast Cancer Can We Find? H.
Gilbert Welch, MD, MPH, and William C. Black, MD Annals of Internal
Medicine December 1997 Volume 127 Issue 11 Pages 1023." Conclusions: A substantial reservoir of DCIS is undetected during life. How hard pathologists look for the disease and, perhaps, their threshold for making the diagnosis are potentially important factors in determining how many cases of DCIS are diagnosed. The latter has important implications for what it means to have the disease. "
(18) http://www.respiratoryreviews.com/apr00/rr_apr00_lungcancer.html
DOES LUNG CANCER SCREENING SAVE LIVES? by Janis Kelly, Respiratory Reviews April 2000.
(19) http://www.bcbsnc.com/services/medical-policy/pdf/lung_cancer_screening_ct_scanning_or_chest_radiographs.pdf
Corporate
Medical Policy Lung Cancer Screening, CT Scanning or Chest Radiographs,
Blue Cross Blue Shield of N Carolina. No Policy coverage for Lung
cancer screening with chest CAT or Xrays.
(20) http://www.annals.org/cgi/content/full/137/5_Part_1/305
The
Canadian national breast screening study. 1. Breast cancer mortality
after 11 to 16 years of follow-up. Miller AB, To T, Baines CJ, Wall C.
Ann Intern Med 2002;137:305 312
"After 11 to 16 years of follow-up,
four or five annual screenings with mammography, breast physical
examination, and breast self-examination had not reduced breast
cancer mortality compared with usual community care after a single
breast physical examination and instruction on breast self-examination.
The study data show that true effects of 20% or greater are unlikely.
Controversy will persist because other studies suggest that screening
causes small reductions in breast cancer mortality."
(21) http://jnci.oxfordjournals.org/cgi/content/abstract/92/18/1490
Canadian
National Breast Screening Study-2: 13-Year Results of a Randomized
Trial in Women Aged 50-59 Years. Anthony B. Miller, Teresa To, Cornelia
J. Baines, Claus Wall, Journal of the National Cancer Institute, Vol.
92, No. 18, 1490-1499, September 20, 2000. "Conclusion: In women aged
50 - 59 years, the addition of annual mammography screening to physical
examination has no impact on breast cancer mortality."
(22) http://www.annals.org/cgi/content/full/137/5_Part_1/344
Screening
for Breast Cancer: Recommendations and Rationale, U.S. Preventive
Services Task Force. Humphrey LL, Helfand M, Chan BKS, Woolf SH. Ann
Intern Med 2002;137:347 -360 The U.S. Preventive Services Task Force
recommends screening mammography, with or without clinical breast
examination, every 1 to 2 years for women aged 40 and older.
(23) http://www.ahrq.gov/clinic/3rduspstf/breastcancer/brcanrr.pdf
United States Preventive Services Task Force concluded mammography reduces breast cancer mortality among women 40-74 years old.
Samuel Epstein MD
(24)(25)(26)(27)(28)
http://www.preventcancer.com/patients/mammography/ijhs_mammography.htm
Dangers
and Unreliability of Mammography: Breast Examination is a Safe,
Effective, and Practical Alternative by Samuel S. Epstein, Rosalie
Bertell, and Barbara Seaman. International Journal of Health Services,
31(3):605-615, 2001. Breast Cancer Coalition.
(25) http://findarticles.com/p/articles/mi_m1525/is_5_84/ai_62896172
Cancer,
Inc and National Breast Cancer Awareness Month. by Sharon Batt, Liza
Gross. Sierra, Sept, 1999" THEY MAKE THE CHEMICALS, THEY RUN THE
TREATMENT CENTERS, AND THEY'RE STILL LOOKING FOR "THE CURE"--NO WONDER
THEY WON'T TELL YOU ABOUT BREAST CANCER PREVENTION". Blistering
Criticism.
(26) http://www.preventcancer.com/work/
Cancer
Prevention Coalition. Samuel S. Epstein, MD founder and Chairman of the
Cancer Prevention Coalition, and is professor emeritus of Environmental
and Occupational Medicine at the University of Illinois School of
Public Health. He has published some 260 peer reviewed articles, and
authored or co-authored 11 books including: the prize-winning 1978 The
Politics of Cancer; the 1995 Safe Shopper's Bible; the 1998 Breast
Cancer Prevention Program; the 1998 The Politics of Cancer, Revisited.
(27) http://www.preventcancer.com/press/books/poc.htm
The
Politics of Cancer, Revisited 1998 By Samuel S. Epstein, M.D. Foreword
by Congressman David Obey, Introduction by Congressman John Conyers In
this book, world-cancer expert Dr. Samuel Epstein indicts the National
Cancer Institute and the American Cancer Society for responsibility in
losing the cancer war.
http://www.stopbreastcancer.org/
Stop Breast Cancer Dot Org
(29) http://jama.ama-assn.org/cgi/content/abstract/288/7/872
Postmenopausal
Hormone Replacement Therapy Scientific Review Heidi D. Nelson, MD, MPH;
Linda L. Humphrey, MD, MPH; Peggy Nygren, MA; Steven M. Teutsch, MD,
MPH; Janet D. Allan, PhD, RN JAMA. 2002;288:872-881.
French Cohort Study
(30) http://www.ncbi.nlm.nih.gov/pubmed/12626212
Combined hormone replacement therapy and risk of breast cancer in a French cohort study of
3175
women. de Lignières B et al., Climacteric. 2002 Dec;5(4):332-40.
French Cohort Study shows no increased risk of breast cancer from
bio-identical human hormones.
DCIS
(31) http://radiology.rsnajnls.org/cgi/content/full/221/3/770
Case
41: Ductal Carcinoma in Situ, by Alanna T. Harris, MD. "The detection
of ductal carcinoma in situ has increased markedly in recent years
secondary to the widespread use of screening mammography, and it now
accounts for 25 to 40% of mammographically detected breast cancers."
(33) http://jnci.oxfordjournals.org/cgi/content/abstract/94/20/1546
Detection
of Ductal Carcinoma In Situ in Women Undergoing Screening Mammography
by Virginia L. Ernster, Journal of the National Cancer Institute, Vol.
94, No. 20, 1546-1554, October 16, 2002. "Conclusions: Overall,
approximately 1 in every 1300 screening mammography examinations leads
to a diagnosis of DCIS. Given uncertainty about the natural history of
DCIS, the clinical significance of screen-detected DCIS needs further
investigation. "
(34) http://www.allbookstores.com/Mammography_p4sd.html
Mammography Books available.
(35) http://www.blogher.com/pink-ribbon-madness-say-no-breast-cancer-exploitation-corporate-profit
Pink Ribbon Madness: Say No to Breast Cancer Exploitation for Corporate Profit by Suzanne Reisman 10/06/2007
(36) http://www.naturalnews.com/022115.html
October is Breast Cancer Propaganda Month: Pinkwashing, Breast Cancer Action and Vitamin D
Thursday, October 11, 2007 by: Mike Adams. Critical of mammography. Advocates checking Vitamin D levels.
NORTIN HADLER. M.D.
(37) http://abcnews.go.com/Health/OnCallPlus/story?id=3196417&page=1
Does Screening Mammography Save Lives? Numbers May Not Justify Practice for Routine Mammograms, OPINION By NORTIN HADLER. M.D.
May 21, 2007, ABC News. Dr. Nortin Hadler is professor of medicine and
microbiology/immunology at the University of North Carolina at Chapel
Hill, and an attending rheumatologist at University of North Carolina
Hospitals.
"In the United States, radiologists are so hesitant
to read a mammogram as "normal" that false positive rates can reach 80
percent. This hedging on the readings is driven by the fact that
"missing a breast cancer" on mammography is the most frequent reason for
malpractice litigation in the United States.
But screening
mammography is so terribly blunt that it approaches useless: It finds
very few cancers that are truly treatable, it misses many of these and
it is awash in false positives. Norway, Sweden, Australia and the United
Kingdom are re-examining their national experience with screening
mammography because of appraisals similar to mine.
If a woman's
life was saved because of early detection of an evil breast cancer, she
should thank her lucky stars rather than her mammographer. I would
relegate mammograms to the archives of false starts, next to radical
mastectomy" Endquote.
(38) http://jnci.oxfordjournals.org/cgi/content/full/92/20/1630
After
40 Years, Mammography Remains as Much Emotion as Science by Judith
Randal, Journal of the National Cancer Institute, Vol. 92, No. 20,
1630-1632, October 18, 2000
"For the better part of a century, it
would have been unthinkable to treat primary breast cancer with anything
but the operation pioneered in the 1890s by William Halsted, M.D., one
of the most prominent surgeons of his day. Beginning in the 1970s, the
Halsted era drew gradually to a close when randomized controlled trials
found that the operation generally known as radical mastectomy was no
more effective than less drastic surgery (sometimes in combination with
radiation). Could a similar fate await the current gold-standard status
of screening mammography? Will a time come when its popularity dwindles,
too?...Mammography now a $4 billion a year industry in the United
States alone...Absent unforeseen developments, it is probably safe to
predict that mammography for screening will continue to be as much about
strongly held opinions and political pressures as about
science."endquote
David Plotkin MD
(39) http://www.theatlantic.com/doc/199806/breast-cancer
Good News and Bad News About Breast Cancer by David Plotkin M.D.
The Atlantic Monthly, June 1998, "Breast cancer is a major
public-health concern; it kills 0.04 percent of all American women
yearly...Most of the time the news is reassuring; two thirds to four
fifths of all biopsies reveal that the abnormality is not malignant.
(Women in their forties are more likely than older women to have
negative biopsies, because mammograms of their naturally lumpier breasts
are harder to interpret.)...An official nationwide mammography program
would be a huge commitment: 51.5 million American women are aged forty
or above. And one must bear in mind the cost of needless medical
procedures generated by the huge number of false-positive
mammograms...two to four false positives for every true positive,
according to some measures.
On balance, then, I reluctantly support
the status quo. When my patients come in for their mammograms, I do not
try to dissuade them. But I tell them that the most optimistic
interpretation of the available evidence suggests that routine
mammography has only a marginal effect on a woman's chances of surviving
breast cancer, and that it may have no effect at all." endquote
(40) http://jco.ascopubs.org/cgi/content/full/21/1/41
High
Prevalence of Premalignant Lesions in Prophylactically Removed Breasts
From Women at Hereditary Risk for Breast Cancer by N. Hoogerbrugge et
al.J ournal of Clinical Oncology, Vol 21, Issue 1 (January), 2003:
41-45. Full text.
"Conclusion: Many women at high risk of
hereditary breast cancer develop high-risk histopathologic lesions,
especially after the age of 40 years. Surveillance does not detect such
high-risk histopathologic lesions."
(41)
http://content.nejm.org/cgi/content/full/348/17/1672?ijkey=809de3fe3d1953b859cb0a1ce2fe8c124442a7f1&keytype2=tf_ipsecsha
Mammographic
Screening for Breast Cancer Suzanne W. Fletcher, M.D., and Joann G.
Elmore, M.D., M.P.H. NEJM Volume 348:1672-1680 April 24, 2003 Number 17
(42) http://www.hsph.harvard.edu/causal/publications/mammography.pdf
POINT
COUNTERPOINT On the efficacy of screening for breast cancer by David A
Freedman, Diana B Petitti, and James M Robins, International Journal of
Epidemiology 2004;33:4355. Review of studies concludes mammography
screening is effective.
(43) http://www.hsph.harvard.edu/causal/publications/rejoinder.pdf
Rejoinder,by
David A Freedman, Diana B Petitti and James M Robins. International
Journal of Epidemiology 2004;33:6973. More on effciacy of screening
mammography.
(44) http://jama.ama-assn.org/cgi/content/full/293/10/1245
Screening
for Breast Cancer. Joann G. Elmore, MD, MPH; Katrina Armstrong, MD;
Constance D. Lehman, MD, PhD; Suzanne W. Fletcher, MD, MSc JAMA.
2005;293:1245-1256. "All major US medical organizations recommend
screening mammography for women aged 40 years and older. Screening
mammography reduces breast cancer mortality by about 20% to 35% in women
aged 50 to 69 years and slightly less in women aged 40 to 49 years at
14 years of follow-up.
Approximately 95% of women with
abnormalities on screening mammograms do not have breast cancer with
variability based on such factors as age of the woman and assessment
category assigned by the radiologist. Studies comparing full-field
digital mammography to screen film have not shown statistically
significant differences in cancer detection while the impact on recall
rates (percentage of screening mammograms considered to have positive
results) was unclear. "endquote
(45) http://cebp.aacrjournals.org/cgi/content/full/13/4/501
Fear,
Anxiety, Worry, and Breast Cancer Screening Behavior: A Critical Review
Nathan S. Consedine, Carol Magai, Yulia S. Krivoshekova, Lynn Ryzewicz
and Alfred . Neugut. Cancer Epidemiology Biomarkers & Prevention
Vol. 13, 501-510, April 2004. "Women's fears surrounding breast cancer
seem to encompass nearly "everything" but certainly include fear of a
breast cancer diagnosis, fear of pain/discomfort, and more complicating,
fear of embarrassment. To this list, we can add fear of the medical
establishment, radiation, nonspecific "cancer worry" general anxiety, or
phobia. " endquote.
Michael Baum
(46) http://www.healthy.net/scr/article.asp?Id=2717
Cancer:
When it isn't a killer DCIS: Precancer, benign cancer or what? What
Doctors Don't Tell You (Volume 13, Issue 10). "The cancer establishment
was recently rocked to its core when Professor Michael Baum, an eminent
and well-respected breast surgeon and researcher, claimed that
screening for breast cancer should be scrapped because it caused
hundreds of healthy women to undergo risky, mutilating and unnecessary
treatments even when they may never develop the disease. His comments,
made at a meeting of the Royal Society of Medicine, cut even more deeply
because Baum was one of the physicians who helped set up the
50-million-a-year breast-screening service (Frith M, Scrap Breast Cancer
Screening, Evening Standard, 10 December 2002, p 1). Baum has
stated publicly that the most dramatic consequence of the rise in the
numbers of routine mammographies has been a huge increase in the
incidence of small, well-contained, relatively benign breast cancers
known as ductal carcinoma in situ (DCIS) (BMJ Rapid Responses at
bmj.com/cgi/eletters/325/ 7361/418#24945, 24 August 2002). " endquote
(47) http://www.bmj.com/cgi/eletters/325/7361/418#24945
Re: Screening and Mastectomy rates, Letter to the editor of BMJ by Michael Baum, Emeritus Prof. of Surgery University College London The Portland Hospital, 212-214 Great Portland Street, London W1W 5QN.
(48) http://www.thisislondon.co.uk/news/article-2407684-details/'Scrap+breast+cancer+screening'/article.do
'Scrap breast cancer screening' By Maxine Frith, Health Correspondent, Evening Standard 10.12.02
The man who helped to set up the NHS breast screening programme claims today that it does more harm than good.
Professor
Michael Baum, a leading expert in the field, said that screening for
the disease causes hundreds of healthy women to have risky, mutilating
and unnecessary treatments even when they may never develop the disease.
Fifteen years after he established one of the first screening
centres in the UK, Professor Baum has now called for the £50million a
year service to be shut. He believes the techniques used for screening
are not accurate enough and lead to too many false alarms.
Professor
Baum, who is to address the Royal Society of Medicine in London today,
has been a long-standing critic of screening but has never before gone
so far as to say it should be scrapped entirely,
He is one of
the most eminent breast surgeons in the country and a respected
researcher into the disease. His comments have sparked a furious row
among experts over the benefits of the NHS breast screening programme
(49) http://news.bbc.co.uk/2/hi/health/6061652.stm
Breast
screen 'wrong care' fears, BBC News, 18 October 2006. "Breast screening
may produce false positives. Concerns have been raised that breast
cancer screening might lead to some women undergoing unnecessary
treatment. Researchers looked at international studies on half a million
women. They found that for every 2,000 women screened over a decade,
one will have her life prolonged, but 10 will have to undergo
unnecessary treatment. UK experts said women over 50 should go for their
breast checks, but a screening pioneer raised doubts about the NHS
programme's future. The report, published in the Cochrane Library,
involved a review of breast cancer research papers from around the
world."endquote.
(50) http://www.telegraph.co.uk/news/uknews/1531694/Doubts-raised-by-the-pioneer-of-screening.html
Doubts raised by the pioneer of screening By Nic Fleming, Medical Correspondent 18/10/2006 .
Prof Michael Baum set up one of the first breast cancer screening programmes in England in 1987.
Cochrane Report
cochrane.org/reviews/en/ab001877.html
Screening for breast cancer with mammography. Gotzsche PC, Nielsen M Cochrane Reviews
Main
results: Seven completed and eligible trials involving half a million
women were identified. We excluded a biased trial from analysis.
Two
(Canada and Malmo)trials with adequate randomisation did not show a
significant reduction in breast cancer mortality, relative risk (RR)
0.93 (95% confidence interval 0.80 to 1.09) at 13 years; four trials
with suboptimal randomisation showed a significant reduction in breast
cancer mortality, RR 0.75 (0.67 to 0.83) (P = 0.02 for difference
between the two estimates). RR for all six trials combined was 0.80
(0.73 to 0.88).
The two trials with adequate randomisation did
not find an effect of screening on cancer mortality, including breast
cancer, RR 1.02 (0.95 to 1.10) after 10 years, or on all-cause
mortality, RR 1.00 (0.96 to 1.04) after 13 years. We found that breast
cancer mortality was an unreliable outcome that was biased in favour of
screening, mainly because of differential misclassification of cause of
death.
Numbers of lumpectomies and mastectomies were
significantly larger in the screened groups, RR 1.31 (1.22 to 1.42) for
the two adequately randomised trials; the use of radiotherapy was
similarly increased.
Authors' conclusions: Screening likely reduces breast cancer mortality.
Based on all trials, the reduction is 20%, but as the effect is lower
in the highest quality trials, a more reasonable estimate is a 15%
relative risk reduction. Based on the risk level of women in these
trials, the absolute risk reduction was 0.05%. Screening also leads to
overdiagnosis and overtreatment, with an estimated 30% increase, or an
absolute risk increase of 0.5%.
This means that for every 2000
women invited for screening throughout 10 years, one will have her life
prolonged. In addition, 10 healthy women, who would not have been
diagnosed if there had not been screening, will be diagnosed as breast
cancer patients and will be treated unnecessarily. It is thus not clear
whether screening does more good than harm. Women invited to screening
should be fully informed of both benefits and harms.
(52) http://www.cochrane.dk/research/Screening for breast cancer with mammography (Cochrane review).pdf
Screening for breast cancer with mammography Gotzsche PC, Nielsen M cochrane collaboration 2006 full text pdf
(53) http://findarticles.com/p/articles/mi_m3225/is_2_68/ai_105645316
Should
we offer routine breast cancer screening with mammography? - Cochrane
For Clinicians: Putting Evidence Into Practice. by Sean P. David.
American Family Physician, July 15, 2003
(54) http://www.bmj.com/cgi/content/full/323/7319/956
Row
over breast cancer screening shows that scientists bring "some
subjectivity into their work Susan Mayor, London, BMJ 2001;323:956 (27
October).
"The review claimed that there was no reliable evidence
to support the value of mammo-graphy screening in reducing deaths from
breast cancer and alleged an association with increased rates of breast
surgery.
Ole Olson and Peter Gotsche from the Nordic Cochrane
Centre, Righospitalet, Copenhagen, Denmark, reassessed as part of a
Cochrane review a meta-analysis of seven randomised trials of screening
mammography which they had previously carried out. This confirmed their
original conclusion, they said, that there was no evidence of a
reduction in either total or breast cancer mortality in two of the
trials that they considered to be of sufficient quality to analyse.
They
added: "We have also confirmed that screening leads to more aggressive
treatment, increasing the number of mastectomies by about 20% and the
number of mastectomies and tumourectomies by about 30%" (Lancet
2001;358:1340-2 )."endquote.
(55) http://www.bmj.com/cgi/content/full/324/7338/677/b
Letters
Breast screening seems driven by belief rather than evidence. Hazel
Thornton, independent advocate for quality in research and healthcare.
BMJ 2002;324:677 ( 16 March )
(56) http://www.bmj.com/cgi/content/full/323/7321/1131/a
Letters.
Office of NHS cancer screening programme misrepresents Nordic work in
breast screening row by Peter C Gotzsche, director. Nordic Cochrane
Centre, Rigshospitalet, DK-2100 Copenhagen ø, BMJ 2001;323:1131 (10
November 2001)
(57) http://www.mammographyed.com/docs/2007/Melbourne-schedule2.pdf
LÃzlo Tabar, M.D. Professor of Radiology Course Director 2007 BREAST SEMINAR SERIES Covering the world of breast diagnosis.
Opposed to Screening
eappleseedproject.org/natbreascanc3.html
National Breast Cancer Coalition (NBCC) The Mammography Screening Controversy:Questions and Answers February 8, 2002
(59) http://www.stopbreastcancer.org//index2.php?option=com_content&do_pdf=1&id=133
Position
Statement on Screening Mammography Updated May 2007. National Breast
Cancer Coalition 1707 L Street, NW, Suite 1060 Washington, D.C. 20036
(202) 296-7477 voice (202) 265-6854 fax
(60) http://www.breastcancerchoices.org/iodineindex.html
BreastCancerChoices.org cancer advocacy Iodine Supplement Information
contact
lynne. Breast Cancer Choices, Inc., a nonprofit organization helping
patients make informed choices about breast screening, diagnostic
procedures and treatment.
(61) http://www.newamerica.net/publications/articles/2002/search_and_destroy
Search
and Destroy, Why Mammograms Are Not the Answer, By Shannon Brownlee,
New America Foundation, The New Republic April 22, 2002
www.jeffreydach.com
www.drdach.com
www.naturalmedicine101.com
www.truemedmd.com
Disclaimer click here: http://www.drdach.com/wst_page20.html
The
reader is advised to discuss the comments on these pages with his/her
personal physicians and to only act upon the advice of his/her personal
physician Also note that concerning an answer which appears as an
electronically posted question, I am NOT creating a physician -- patient
relationship. Although identities will remain confidential as much as
possible, as I can not control the media, I can not take responsibility
for any breaches of confidentiality that may occur.
Link to this article:
http://jeffreydach.com/2007/11/04/the-untold-message-of-breast-cancer-awareness-month.aspx
This article may be copied or reproduced on the internet provided a link and credit is given.
(c) Copyright Jeffrey Dach MD 2008-2009 All Rights Reserved
